The infants response to the pull--to-sit maneuver is often used as a test when assessing motor development. It provides a good measure of the infant's neck muscle strength as well as the development of effective anticipatory postural responses.
Newborn
When pulled to sit, the head lags behind the body, but does not fall back fully. Once the trunk is erect, the infant will lift the head in line with the trunk.

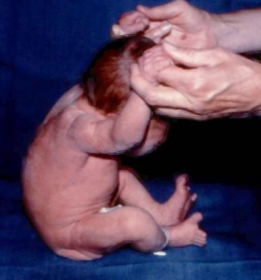
Will 10 weeks
The PTS maneuver is often used to assess infant motor abilities; the infants forearms are grasped and the infant is pulled up from supine into sitting. At 10 weeks Will anticipates the movement of the head when pulled to sit, and is able to maintain the head in line with the trunk as the PTS maneuver proceeds.

Once the trunk is upright and tilted forwards a little Will is able to hold the head in line with the trunk. He is also able to lift the head erect to look at me.
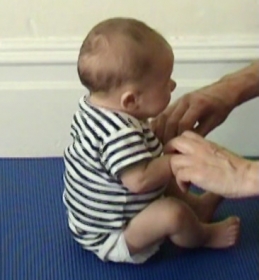

In the video clip you see me pulling Will up 5 times. By the fifth repeat Will's neck muscles have started to tire and he is not able to keep the head in line with the trunk at the beginning of the PTS maneuver.
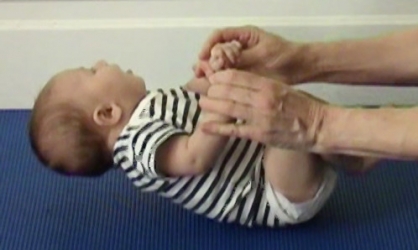
When supported in sitting, Will is able to maintain his head erect for extended periods of time, and is able to rotate the neck with varying degrees of head on neck flexion depending on the direction of his looking.



When pulled to sit Will actively flexes his neck as well as his trunk and UE flexors.



When lowered from sitting to supine, Will actively flexes the neck.


Will 4 months (22 weeks)
At 4 months Will anticipates the being pull into sitting and once the head is lifted up off the support surface he activity lifts himself by flexion the shoulders and elbows. The trunk flexor muscles are engaged and the LEs lift up off the SS. Once his trunk is erect Will extends the neck to look at me.





In this next sequence you see how Will activity participates in controlling the the head and trunk and he is lowered from sitting to supine. He does this by engaging the abdominal muscles and neck flexors to stabilize the trunk and head, while at the same time controlling elbow extension with eccentric contraction of the shoulder and elbow flexors.





Flanagan JE, Landa R, Bhat A, Bauman M. Head lag in infants at risk for autism: a preliminary study. Am J Occup Ther. 2012 Sep-Oct;66(5):577-85. doi: 10.5014/ajot.2012.004192. PubMed PMID: 22917124. PDF via Researchgate
Pineda, R. G., Reynolds, L. C., Seefeldt, K., Hilton, C. L., Rogers, C. L., & Inder, T. E. (2016). Head Lag in Infancy: What Is It Telling Us? The American Journal of Occupational Therapy, 70(1), https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4690596/
OBJECTIVE. To investigate changes in head lag across postmenstrual age and define associations between head lag and (1) perinatal exposures and (2) neurodevelopment.
METHOD. Sixty-four infants born ≤30 wk gestation had head lag assessed before and at term-equivalent age. Neurobehavior was assessed at term age. At 2 yr, neurodevelopmental testing was conducted.
RESULTS. Head lag decreased with advancing postmenstrual age, but 58% (n = 37) of infants continued to demonstrate head lag at term. Head lag was associated with longer stay in the neonatal intensive care unit (p = .009), inotrope use (p = .04), sepsis (p = .02), longer endotracheal intubation (p = .01), and cerebral injury (p = .006). Head lag was related to alterations in early neurobehavior (p < .03), but no associations with neurodevelopment were found at 2 yr.
CONCLUSION. Head lag was related to medical factors and early neurobehavior, but it may not be a good predictor of outcome when used in isolation.
Reddy, V., Markova, G., & Wallot, S. (2013). Anticipatory Adjustments to Being Picked Up in Infancy. PLoS ONE, 8(6), https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3688725/